Our team was thrilled to participate in the 4th African Conference on Emergency Medicine this…
GECC and The Future Of Emergency Care In Uganda
Written by: Omeed Saghafi, MD, GECC volunteer
When you have an emergency in the United States, you go the Emergency Department (ED). If you are truly sick with a life threatening emergency, you will probably be seen by someone like me, a board certified Emergency Physician within minutes of your arrival to the ED.
In Uganda, patients experiencing an emergency have much more difficulty accessing this life saving care. In Uganda, if you have an emergency, you need to find a ride to the hospital. If you’re lucky, the hospital will have an “Emergency Department” where you wait until a provider (who likely has no training in the specialty of emergency care) can see you. You will either receive minor treatment and be discharged or be admitted to the hospital with treatment expected to occur “on the ward.” Then, you wait some more. According to the statistics, you will wait an average of 26 hours to be seen by a doctor. You may die waiting, but this is the best option in a country with limited resources.
“But, you would be amazed how the right teaching, and even the most simple of tools in the right hands can change how a country cares for its people.”
A few months ago, I decided to volunteer with the Global Emergency Care Collaborative (GECC), a nonprofit organization dedicated to increasing access to emergency care in low resource settings. GECC’s founders believe that treating acutely injured patients with trained providers can save many lives. Many unnecessary deaths can be prevented with timely emergency care. Even with limited resources, GECC has developed a model for a country to provide emergency care to its people. GECC has developed a program to build capacity for both emergency care delivery and training in places where no trained emergency care providers exist.
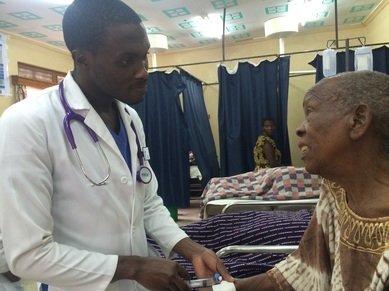 Many countries in sub-Saharan Africa, including Uganda, have physician shortages. To combat this, GECC trains the best, local nurses to become non-physician clinicians specialized in Emergency Care, called Emergency Care Practitioners (ECPs). These ECPs are similar to Nurse Practitioners in the US, but they receive focused specialty training in Emergency Medicine on how to care for the sickest patients and do so quickly. Board-certified Emergency Physicians train and mentor the first class of ECPs. Afterwards, GECC focuses on building local capacity to carry out the training, thus creating a sustainable model to build emergency care capacity. GECC also supports physician training in emergency medicine as a necessary compliment to the training and skills of the ECPs. Ultimately, the graduated ECPs and local emergency physicians can assume control of the emergency care training and emergency departments through the country. While this capacity continues to develop, the GECC of emergency physicians is constantly available to help with mentoring, logistics, and other resources as needed, visiting the sites frequently.
Many countries in sub-Saharan Africa, including Uganda, have physician shortages. To combat this, GECC trains the best, local nurses to become non-physician clinicians specialized in Emergency Care, called Emergency Care Practitioners (ECPs). These ECPs are similar to Nurse Practitioners in the US, but they receive focused specialty training in Emergency Medicine on how to care for the sickest patients and do so quickly. Board-certified Emergency Physicians train and mentor the first class of ECPs. Afterwards, GECC focuses on building local capacity to carry out the training, thus creating a sustainable model to build emergency care capacity. GECC also supports physician training in emergency medicine as a necessary compliment to the training and skills of the ECPs. Ultimately, the graduated ECPs and local emergency physicians can assume control of the emergency care training and emergency departments through the country. While this capacity continues to develop, the GECC of emergency physicians is constantly available to help with mentoring, logistics, and other resources as needed, visiting the sites frequently.
GECC’s innovative model is not a medical mission. It is not a two-week trip to a remote village where foreigners do surgery, hand out medications, and then leave a small group of people no better off between visits. This is a unique example of sustainable International Medicine at its best. This is a way to change how medicine is delivered across an entire country.
The ECP training program began as a trial in a rural district hospital, called Nyakibale in southwestern Uganda. The program has succeeded and is now being expanded to a large government hospital in the city of Masaka. Concurrently, GECC is working with the Ugandan government to integrate the ECP cadre and Emergency Medicine into the national medical education system and create a standard of care across the country.
Yes, the resources are still limited. Sometimes the ECPs are lucky to even have their own stethoscope and a functioning blood pressure cuff. But, you would be amazed how the right teaching, and even the most simple of tools in the right hands can change how a country cares for its people.



This Post Has 0 Comments